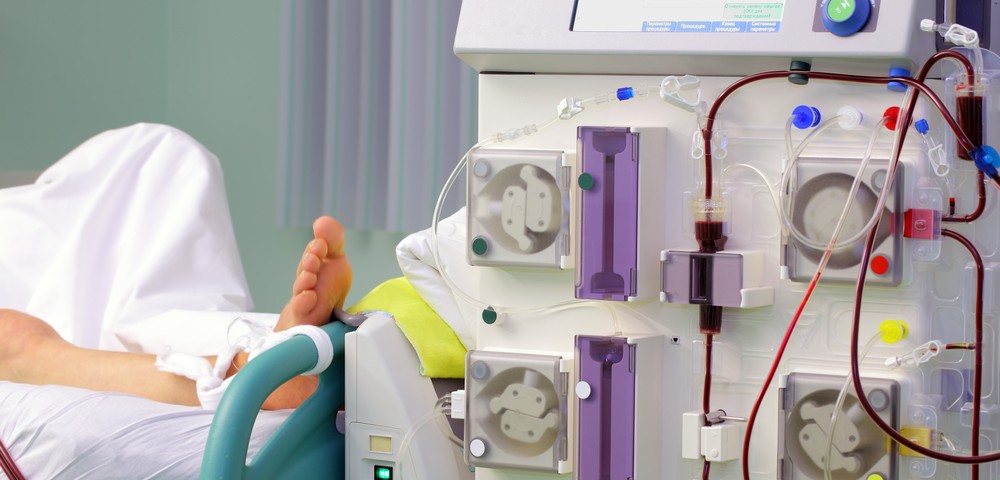
Significant risk factors for pneumonia linked to drug-resistant pathogens in a healthcare setting — including in patients undergoing kidney dialysis, or hemodialysis — are advanced age, more severe pneumonia, and wound care, researchers reported.
The study, which included as a specific group people undergoing kidney dialysis (hemodialysis), is titled “Risk factors to predict drug-resistant pathogens in hemodialysis-associated pneumonia,” and published in BMC Infectious Diseases.
The concept of healthcare-associated pneumonia (HCAP) was introduced by the American Thoracic Society/Infectious Disease Society of America (ATS/IDSA) in 2005, and recommended the use of broad spectrum antibiotics as treatment. The researchers, however, suggest such antibiotic use might worsen the problem of drug resistance in dialysis and other patients.
Hemodialysis-associated pneumonia (HDAP) is a dangerous and frequent complication in dialysis patients, with one U.S. study finding that about one-third of these patients were diagnosed with pneumonia during a five-year period. But the whether hemodialysis is a risk factor for drug-resistant bloodstream infections is a point of controversy among researchers, with some finding a link and others not. According to the societies, however, HDAP can be considered as a part of HCAP.
In this retrospective study, researchers focused on identifying risk factors for these pathogens, and on the demographic and clinical characteristics and microorganisms shared by HDAP and HCAP. A total of 530 patients diagnosed with HCAP were included, of whom 48 (9.1 %) were undergoing regular hemodialysis.
Researchers identified Pseudomonas aeruginosa and methicillin resistant Staphylococcus aureus (MRSA) as the most common pathogens in the dialysis group. These patients were also significantly younger than those with HCAP who were not on dialysis, and had less severe cases of pneumonia. While the incidence of diabetes mellitus was higher in the dialysis group, the non-dialysis group had more comorbidities, such as cerebrovascular illnesses, malignancy, and chronic obstructive pulmonary disease.
The incidence of drug resistant pathogens was not significantly different between the two groups. The researchers identified care of wounds (resulting, for example, from dialysis or chemotherapy), severe pneumonia, and more advanced age (older than 70) of more than 70 years as significant risk factors for drug-resistant pathogens in patients with healthcare-associated pneumonia. Such results indicate that while dialysis and non-dialysis patients had heterogeneous clinical characteristics, they had similar patterns of pathogens.
“In spite of the small sample size, our results provide additional information with regards to the pathogens than large-scale retrospective studies that did not mostly identify causative pathogens,” the researchers concluded. “Taking these [risk factors] into consideration, the unnecessary use of broad spectrum antibiotics may be avoided.”